Justification and optimisation
In medicine, use of radiation must be justified
The ‘Justification and Optimization » principles are part of the European directives included in the regulations of the Union member countries. These two radiological protection principles play an important role especially in the medical field responsible today for 98% of exposures to non-natural sources of radiation.
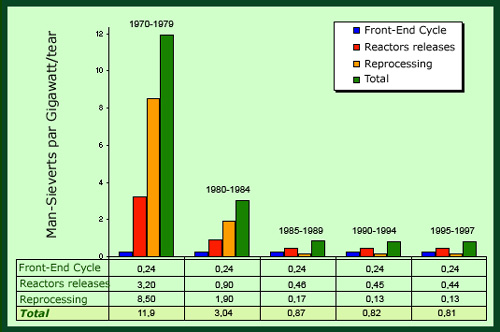
Optimization in nuclear industry
Optimized procedures nuclear industry have reduced by more than 10 in thirty years the radiation exposures of populations, as can bec seen from the evolution of the local and regional collective dose received by the public. Considering that a gigawatt of power supplies electricity to about one million people in France, the individual exposure to radioactivity of a person due to power plants operations and the « uranium cycle » is now below one millionth of a sievert, that is about one-thousandth of exposures coming from health-care.
© IN2P3 (Source UNSCEAR)
These principles intervene also in industry where radioactive techniques should be used only if they provide a benefit over other methods. In the nuclear industry, optimization has reduced exposures to radioactivity to the point that it represents only 1-2% of the medical exposures. It is at the origin of even more dramatic advances in radiological protection of staff exposed to radioactivity.
In medicine, justification consists to irradiate only if really useful information can be expected for the care of the patient. For example, one would prefer a not irradiating Magnetic resonance imaging (MRI ) to a scanner (X-ray computed tomography) every time the scanner does not provide an added benefit.
When radiation is used in medicine, optimization means that one should irradiate with the maximum efficiency, while minimizing the intensity of radiation and the dose received.
Given the little knowledge we have about the effects of low doses, one should avoid to overlook eventual effects. One should avoid, in the opposite direction, the trap of an excessive fear of radiation which could be detrimental to medical diagnosis and cares : Any dose as low to one millisievert or one tenth of a millisievert does not present a serious risk for a patient.
The justification and optimization rules required by European directives are justified by the fact that it is not possible to exclude an effect of low doses. However, some radioprotection experts believe that low dose effects may be much smaller than those assumed by the regulations which are based on the « linear no threshold » model, in which case the dose limits, would actually be very conservative.
The younger a person is, the more justification and optimization are necessary. A 10 millisieverts dose for a 50 years old man is probably unimportant, but the same dose applied to a very young subject, especially to infants, may have consequences. This is shown for instance by the increase by a factor of 5 to 10 of the young children thyroid cancers risk, while the risk may be null beyond 20 or 30 years.
These examples of precautions to take for young children incline to command caution and common sense. The consequences of radiation exposure depends on many factors and one should be wary of oversimplifications and misleading generalizations.
Learn more :
Other articles on the subject « Radioprotection »
Radioprotection principles
Applying common sense rules according to radiation nature The need for protection from radiation [...]
Gamma Radioprotection
A penetrative radiation more difficult to absorb In the case of ingestion of radioactive substanc[...]
Gamma Attenuation
Attenuation of a gamma beam Of the three types of radiations, gamma rays are the most penetrative[...]
Gamma Absorption
Heavy materials for the absorption of gamma rays In terms of radioprotection mitigate gamma rays [...]
Radioprotection neutrons
A rare radiation, dangerous, penetrating, difficult to absorb The neutron radiation is more penet[...]
Radioactive Decontamination
Avoid all contact, ingestion and inhalation One of the tasks of radiation protection is the decon[...]
Reglementations and controls
Strict regulations for an efficient radioprotection Radioprotection has a long history. Its princ[...]
Dose legal limits
Applying the precautionary principle and setting cautious limits French regulations set at 1 mSv [...]
Actors in radioprotection
The actors and the basics of radioprotection regulations The rules of radiation protection are no[...]