Uses of radioactivity in diagnostic medicine : The functionning of living organisms
The use of radioisotopes in medicine has enabled us to acquire a greater understanding of the inner functionning of our body. The visualisation techniques that are now common in diagnostic medicine have given us both a more extensive knowledge and a more effective capacity to heal.
Scintigraphic examinations use the scintillations produced by gamma photons in certain crystals, hence the name of scintigraphy which is commonly given to them.
For the diagnosis, thanks to the injection of the radioactive tracer in vivo, the nuclear physician can access a functional and metabolic imaging. This allows the detection of the serious lesions, the monitoring of their evolution as well as the follow-up of the surgical interventions when necessary. Two existing techniques are gamma scintigraphy and positron emission tomography.
Scintigraphic examinations are carried out in the nuclear medicine departments of hospitals and clinics.

Gamma camera scintigraphy
Gamma-camera detect emitted gamma photons : These common device in nuclear diagnostic, provides a functional image of an organ after administration to the patient of a specific tracer, such as thallium-201 for the myocardium. Radioactive atoms emit photons captured by two planar detectors placed at 180 ° or 45 depending on the examination. The scintigraphies are routine clinical examinations that provide diagnosis, help to therapeutic decisions, disease evaluations and prognosis.
© CEA – L.MEDARD(SHFJ)
In 2016 the number of people using nuclear medicine was estimated to 35 million, either for a diagnosis or for a therapy. The demand for radioisotopes for these diagnoses and therapies is increasing worldwide, both in developed and fast-developing countries like China and India.
In 2017, France had 750 specialist doctors in more than 200 nuclear medicine centers. The number of diagnoses made, mainly scintigraphies, was 1.5 million, an increase of 9% per year.
Nuclear medicine departments hold specific authorizations from competent authorities for the medical use (diagnosis or therapy) of unsealed radioactive sources and are therefore subject to strict radiation protection regulations.
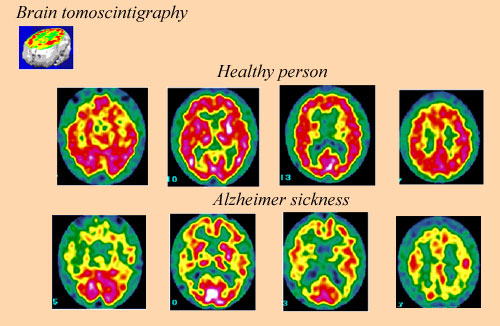
Exploring the brain
Scintigraphy is a commonly used techniques in understanding the way the body works, and providing diagnostics when it doesn’t. The level of the radioactive tracer present in the brain is directly proportional to the rate of blood flow: it is at a maximum in the most active parts of the brain (coloured in red). This comparison of brain ‘slices’ for a healthy person and an Alzheimer victim helps to highlight the affected areas, showing that damage is done in active sections of the brain
© André Aurengo, Hôpital Pitié-Salpétrière
The ‘tracer method’ – a crucial component of the above-mentioned techniques – was first developed by Georg von Hevesy in 1923. It was not until 1934, however, when Irene and Frederic Joliot-Curie pioneered the creation of artificial radioactive isotopes, that doctors and biologists were first able to use the tracer method in making their diagnoses.
Advances made over the last eighty years have meant that much weaker forms of radiation, which make for more accurate and delicate scans, can also easily be detected. This means that radioactive sources can now be taken into the body without damaging the healthy tissue. As a result, doctors can have patients ingest specific radioactive samples which will either follow certain processes in the body or attach themselves to certain organs. The radiation emitted by these sources can be analyzed to reveal information about the way the body works: such elements are known as radioactive or radiopharmaceutical ‘tracers’.
Towards the end of the 1940’s, iodine 131 was first used as a radioactive tracer. The body tendency to absorb iodine into the thyroid gland made iodine 131 an excellent tracer for thyroid cancer, and marked an important milestone in the history of radioactivity in medicine.
The real-life applications of the tracer method are numerous and varied: phosphates marked with technetium 99 are used in bone tissue scans, myocardial scintigraphs are carried out with thallium 201, thyroid scintigraphy involves iodine 123 and lung scans frequently use krypton 81. These scans, often carried out with gamma cameras, provide information that is invaluable to doctors in choosing the appropriate therapies.
In order to make a safe and efficient scan of the brain, lighter radioactive tracers need to be used. The use of positron emitters (oxygen, fluorine…) in positron emission tomography (or PET scanning) allows for the specific targeting of lighter molecules to serve as tracers. This technique has truly revolutionized oncology by allowing for the identification of tumours at a much earlier stage than was previously achievable.
The applications of radioisotopes are not just limited to imaging, however. Beta emitters are frequently used for therapeutic purposes, for both curative and palliative ends (metabolic radiotherapy is a good example of the latter). In the field of therapy, the radioactive product can destroy cancer cells by generating high doses of radiation. Thanks to the targeted injection of radiopharmaceutical drugs, it is possible to treat, for example, certain cancers such as hyperthyroidism and synovitis.
Articles on the subject « Scintigraphic examinations »
Nuclear Scintigraphies
A range of diagnoses for determining how the body works … The word ‘scintigraphy&lsqu[...]
Scintigraphic Diagnostics
A tool for non-aggressive analyses of biological functions Diseases are biological processes and [...]
Indications for Scintigraphy
When to Use Scintigraphy? The nuclear medicine physician must choose the appropriate marker produ[...]
Bone Scintigraphies
Principle and implementation of bone scintigraphies Bone scintigraphy is based on the fixation in[...]
Cardiac scintigraphies
Investigations of the cardiac muscle functionning MYOCARDIAL SCINTIGRAPHY BY PERFUSION Principle [...]