Can effects caused by low doses of radiations be predicted ?
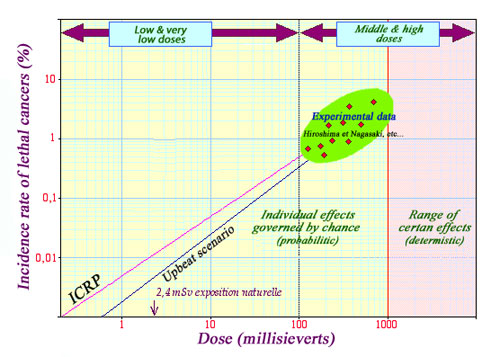
Estimation of cancer risk for small doses
The biological effects for weak doses of radiation are both too small and too dominated by the laws of chance to be measured. This lack of data has prompted the ICRP to propose that the effect varies proportionally with the dose. The relationship becomes a straight line passing through the origin and the closest possible to the actual data points available. The graphs can be used to deduce a likelihood of 5% rate of developing a fatal cancer per sievert. A logarithmic scale is necessary to represent doses and effects over several orders of magnitude.
© IN2P3
Even though we are constantly exposed to weak doses of both natural and man-made radiation, there is still insufficient data for us to be able to accurately evaluate the effects of such an exposure. Empirical but fairly vague predictions have to be made about doses of the order of hundreds of millisieverts (mSv), and anything smaller than that is even less clear.
(mSv), and anything smaller than that is even less clear.
Despite the absence of hard data, experts have done their best to evaluate how dangerous weak sources of radiation can be. As a necessary step in the journey to effective radioprotection, a number of different predictive models have been drawn up which attempt to prove a causal link between weak doses and biological effects.
In the field of especially weak effective doses all effects are known as ‘probabilistic’ – which implies that random chance or bad luck plays a dominant role between individuals. In the very great majority of cases this random chance works to our advantage, and our bodies are able to repair most of the damage such weak rays can do. If for whatever reason these reparations cannot take place, then cancers or even genetic mutations may manifest themselves within a few years. However there is no scientific proof that very low doses generate cancers. This is simply an assumption.
Where this level of exposure is concerned, it is the probability and not the severity of risk that increases with the dosage. Where individuals are concerned, it is almost impossible to link the appearance of a cancer with exposure to radiation.
The official model adopted by the ICRP (International Commission on Radiological Protection) describes a simple linear relationship between the probability of an effect (such as the appearance of a cancer) and the dosage involved. On a graph representing the effect as a function of dosage, the relationship is represented by a straight line passing through the origin. The probability therefore grows in proportion to the increase in dose.
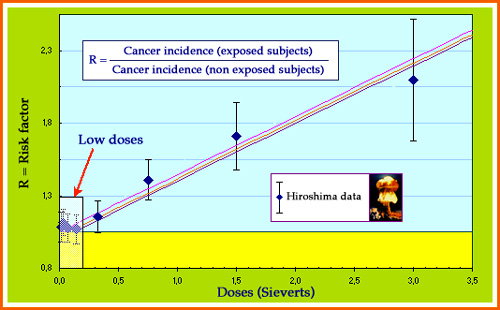
Scarce data and large uncertainties
The data available to establish the dose-effect relationships are rare and comes with substantial error margins. The main data sets currently available, are taken from the irradiated survivors of Hiroshima and Nagasaki. The error bars associated to a data point means that the real risk value has a 70% likelihood of falling within the bar. At small dose values the uncertainties are so large that it is impossible to explicitly discriminate between the three proposed models drawn on the plot.
© IN2P3
The important value to measure is the slope of this line – the constant of proportionality. With data being (fortunately) rare, experts in the field of radioprotection have had to base their assumptions entirely on case studies of those irradiated in Hiroshima and Nagasaki.
The probability of a cancer being induced by radioactivity has thus been estimated at 5% for every additional sievert. Applying these statistics to the current French population of 60 million, natural radioactivity taken in conjunction with medical scans (which average between 1 and 2.5 mSv per year and inhabitant) will cause between 3,000 and 7,500 of the 120,000 deadly cancers diagnosed annually. With no biological label on these cancers to identify their original causes, all calculations involve a certain degree of speculation.
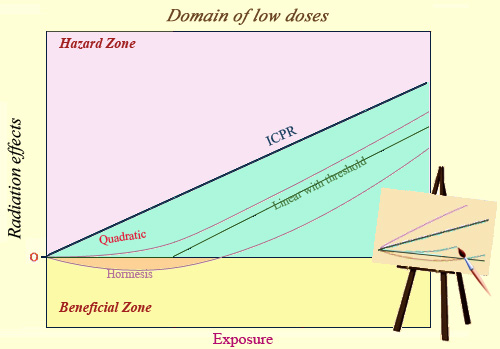
Incertitude about models …
In the range of weak doses (below 200 mSv), the relationship between dose and effect is not known. The absence of reliable data makes accurate prediction difficult. A range of alternatives to the ICRP model are possible. Two popular alternatives are a linear relationship with a lower bound below which radiation produces no effect, or a low-dose region where an effect known as ‘hormesis’ means that low doses might conceivably have beneficial medical effects.
© IN2P3
Even with surveys covering millions of people, it is almost impossible to pick out a definite trend caused by low doses of radioactivity.
The absence of evidence has led many specialists to cast doubt over the reliability of the aforementioned model, believing that it exaggerates the potential dangers. Is there a dose limit below which radiation is no longer toxic? Would the damage be erased by our cells ability to heal themselves?
We are not equal before ionizing radiation. Advanced laboratory techniques such as immunofluorescence confirmed in the field of medical imaging (ie for low doses of a few mSv) that the sensitivity of cells DNA to radiation varied from individual to individual. For example, the DNA radiosensitivity was found more pronounced in patients having a familial risk of breast cancer than in those without this risk identified in their family.
The uncertainty surrounding these weak doses is often ignored by official legislation, which fixes minimum legal exposures as though the values are written in stone. The models in use all involve great simplifications and neglect such crucial factors as the exposure rate and age of the exposed individuals.
NEXT : Dose rate
Other articles on the subject « Radiation Effects »
Deterministic effects
The domain of strong doses and severe, reproducible effects For high doses above a certain thresh[...]
Probabilistic effects
The domain of low and average doses For weak or medium-strength doses, the effects are not as cle[...]
Cumulative Dose
What is the cumulative exposure? We receive an average of 2.5 millisieverts (mSv) per year from n[...]
Dose Rate
Acute and chronic exposures The « effective dose » is not sufficient by itself to characterize on[...]
Hiroshima Nagasaki Survivors
An exces of cancers and leukaemia among survivors Our knowledge of the risks of cancers due to ra[...]
Linear No-threshold Model
A Precautionary Principle applied to radioactivity … Is it possible to predict the effects [...]
Low doses effects
Do low doses of radiation have any effect? Radioprotection experts commonly refer to doses below [...]
Radiosensitivity
Sensitivity of DNA in living cells to radiation Although we still know little about the effects o[...]
Radioactive Toxicity
A useful indicator but to be used appropriately … The danger presented by a radioactive sub[...]
Dose Factors
What doses when swallowing or inhaling radioactive atoms ? How to evaluate the doses resulting fr[...]