From radioactive indicators to CT, scintigraphy and PET …
The name of Georg de Hevesy is associated with the beginnings of radiodiagnostics. In 1913 returning at the Radium Institute in Vienna, after his stay at the Rutherford laboratory, the Hungarian chemist developed with Friedrich Paneth a method using radioisotopes as tracers in chemical reactions. Since he had found that chemistry was powerless to differentiate lead from « radium-D, » Hevesy thought that biological systems would not succeed either.
He used this radium D, actually a radioactive isotope of lead, to explore the absorption of this element by plants. He soaked the root of some plants in a solution of lead and radium D nitrate, and then, measuring the radioactivity acquired, he showed that most of the lead passed through these roots. A few years after that anecdote, it is in 1924 that goes back the first use of the indicators in the man. Two American doctors, Blumgart and Weiss, injecting radium C (Bismuth-214) into one arm, measure the speed of circulation of blood between one arm and the other arm, as well as the variations of this blood circulation speed in cardiac patients.

1971 : Scanner and image reconstitution
The first scanner with image reconstruction is due to the English engineer Godfrey Hounsfield. The mathematics of the reconstruction of tomographic cross-sectionsis due to the South African physicist Allan Cormack. On October 1, 1971, the scanner entered medical practice with the first brain image of a patient at Wimbledon’s Atkinson Morley Hospital. In 1975, Hounsfield built a full-body scanner. Godfrey Housfield and Allan Cormack received the Nobel Prize
© Vanderbilt.edu
What then hampers the development of the method was the small number of natural radioelements available! In 1934, Irene and Frédéric Joliot-Curie demonstrated the possibility of creating radioactive isotopes of any element whereas it was necessary to use until then the rare descendants of uranium and thorium. Thus was discovered in 1937 by Emilio Segre the Technetium, the element No. 43 then missing the table Mendeliev. Technetium-99m is today the radioisotope most used in nuclear imaging because it emits only gamma rays. In the 1960s, the development of a technetium-99m generator contributed enormously to the development of scintigraphy by making the precious radioelement available in hospitals.
The utilization of radioelements became the basis of functional exploration and the origin of valuable diagnostic techniques. Functional imaging techniques would focus on the function of organs, tissues or cells, that is, their metabolism. Functional imaging techniques are scintigraphy, positron emission tomography (PET) with or without a scanner (PET-SCAN) associated.
This development of nuclear imaging would not have been possible without the decisive progress that has occurred in parallel in the field of medical imaging in general, particularly with the invention in 1970 of CT by English engineer Godfrey Hounsfield who revolutionized radiology and more generally imaging.
Initially the X-rays pictures were only projections where all the tissues encountered are superimposed. By the 1920s, attempts had been made to obtain cross-ections at a specific depth, using various tomographic methods. But it was thanks to the independent works of Allan Cormack (1924-1998) who establishes the theory and Godfrey Hounsfield (1919-2004) and to the developments of computational calculations that one passed from these cross-sections to the reconstitution of images in the space.
In the first scanograph (or scanner) a narrow X-ray beam was generated that was received by a detector. The attenuation of the beam was measured along this beam direction. Transmitter and receiver turned together around the body. The exposures were long. From the attenuations observed during this rotation, the attenuation caused by each of the small elementary volumes in the body traversed by the beam was calculated. These digital data were transformed into an image, a true anatomic (tomographic) section of the body. It is the computer revolution and the arrival of more and more powerful, fast and means of computation available on site that allow these very complex reconstructions.
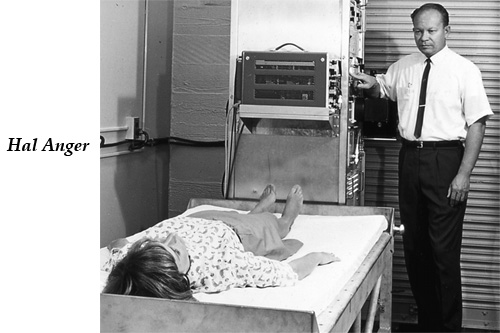
First scintigraphies
Hal Anger (1920-2005) was an engineer and biophysicist inventor of the scintillation camera in 1957. He is considered one of the pioneers of nuclear medicine. His gamma camera developed in the 1950s in Berkeley, produced an image of the metabolic processes at work in organs, tissues and cells, especially in case of disease.
© DR
1958: The Anger Gamma Camera and the first scintigraphies in the United States
Scintigraphy was the first to be developed from the 1950s, following the Hal Anger’s gamma camera. This is now by far the most widely used nuclear medicine diagnostic tool.
While in a radiograph, the X-ray beam passes through the body and there are differences in absorption, in nuclear imaging, radiation is emitted by the tissue that has selectively fixed radioactive isotopes. To establish a diagnosis, it is necessary both to detect the emitted radiation and to reconstitute the concentrations of these radioactive tracers in the body of the patient. The development of scintigraphy is due both to the progress of detection techniques and to the computer techniques of computation allowing these reconstructions.
The first attempts to obtain interpretable images date from the 1940s to the 1950s. The apparatus was based on the principle of scanning scintigraphy, a probe moving on the surface of the body while a marker stylet mechanically controlled by this probe movement reproduced on paper some gray levels depending on the amount of radioactivity detected. These systems were heavy, very slow and the definition of the image rudimentary.
It was in 1956, in Berkeley, California, that the American physicist H. Anger built the scintillating camera and perfected this scintigraphic camera whose principle is still the basis of the current instruments. A scintillating crystal (hence the name « scintigraphy » given to examinations made by this method) transforms the energy of the gamma photons, coming from the body of the patient, into light. The coordinates of the luminous points scattered around the crystal are identified by a battery of photomultipliers and reproduced on a screen where the contours of the distribution of the radioactive tracers in the organism are outlined.

Development of positron emission tomography
The first PET camera for medical applications was built by Hoffman, Michel M. Ter-Pogossian, and Michael E. Phelps in 1973 at the University of Washington. The first full-body scanner appeared in 1977. Today there are more than 400 PET-Scans worldwide.
© A.Aurengo
Later, Positron Emission Tomography (PET) was developed in 1975. The first concepts date back to the work of David E. Kuhl, Luke Chapman, and Roy Edwards in the late 1950s, which led to the design and development of construction of first tomographic prototypes at the University of Pennsylvania. Tomographic imaging techniques were then developed by Michel Ter-Pogossian, Michael Phelps et al. at the University of Washington School of Medicine. As for scintigraphy, a decisive factor for the diffusion of Positron Emission Tomography (PET) was the development of a suitable radiopharmaceutical tracer, fluorine-18 (FDG), at Brookhaven (Al Wolf and Joanna Fowler). Then it was the computer revolution and the arrival of more and more powerful, fast and delocalized computing resources that allow these very complex reconstructions. These computational techniques are used in scintigraphy to establish the distribution of radioactive tracers in tissues.
Multiple devices and techniques (radiation collimation, spectrometry to select the desired precise energy, processing of the raw image, etc.) aim to improve the quality of the images. Scanned images are stored in computer memories. Thanks to the internet they are also immediately available to the teams doctors for further diagnosis and treatment.
Learn more :
Discovery of artificial radioactivitysotopes
Other articles on the subject « Nuclear Imaging »
Gamma Cameras
The most widespread of nuclear medical diagnostics Gamma cameras or scintillation cameras are pie[...]
Gamma-camera : principles
Detect gamma rays and reconstruct their line of flight The emission of a single gamma ray is a ve[...]
Positron Emission Tomography
PET : an instrument for early cancers detections Positron emission tomography, or PET, is a techn[...]
PET : Principles
Simultaneous detection of two annihilation gamma photons Positron Emission Tomography is an imagi[...]
PET Scan
Fruitful combination of two medical imaging techniques One of the latest technological advances i[...]